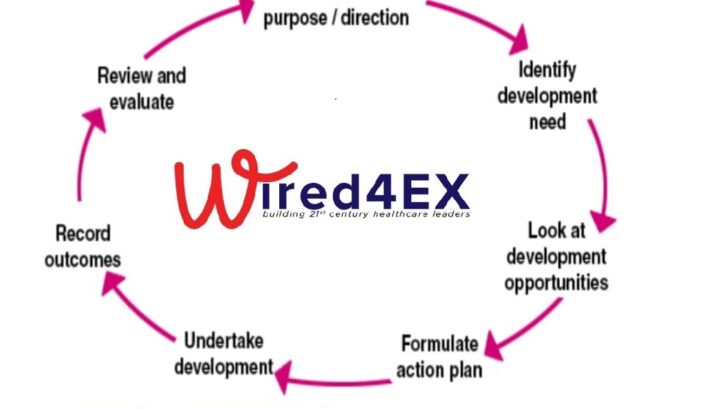
Are you passionate about healthcare management and eager to make a difference? The Wired4EX Program is on a mission to mentor 4,500 healthcare managers, and we need YOU to be part of this transformative journey!
Why Join Wired4EX?
🔹 Mentees: Enhance your skills with our skill-based courses, gain valuable insights from experienced mentors, and earn certificates and continuous development points (CPDs).
🔹 Mentors: Share your expertise, guide the next generation of healthcare managers, and contribute to the growth of the healthcare sector.
🔹 Supporters: Help us promote the program, recruit trainers and trainees, and support our initiatives to strengthen healthcare systems.
🔹 Donors: Your contributions will enable us to provide high-quality training and mentorship, ensuring the success of our program and the development of skilled healthcare managers.
🔹 Facilitators: Lead boot camps, workshops, and events, and play a crucial role in the professional development of our participants.
Get Involved:
👉 Become a Mentor or Trainer: Share your knowledge and experience to guide healthcare managers on their professional journey. If you have accumulated 5 or more years and are in Mid or senior level you can express your interest to mentor by writing to the coordinator info@hesma.or.ke
👉 Enroll as a Mentee: Take advantage of our comprehensive training and mentorship opportunities to advance your career. Cohort is ongoing currently. We are admitting April 2025 (Cohort #10 NOW!)
👉 Support the Program: Promote Wired4EX within your network and help us reach our goals.
👉 Donate: Contribute to the success of the program and the development of future healthcare leaders.
👉 Facilitate Events: Lead engaging and impactful boot camps and workshops.
Join us in making a lasting impact on the healthcare sector. Together, we can drive positive change and build a stronger, more resilient healthcare system.
🔗 Learn more and get involved: https://wired4ex.co.ke/
Let’s make a difference, one healthcare manager at a time! 🌍💙
hashtag#HealthcareManagement hashtag#Mentorship hashtag#ProfessionalDevelopment hashtag#Wired4EX hashtag#JoinTheMovement
Peter Korzenik Fredrick Kimemia FeHSM Rachel Waireri, PhDc, MBA, MHA